|
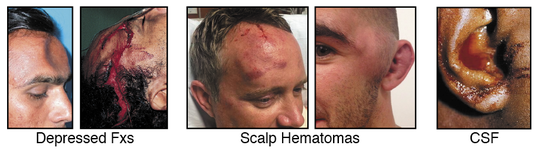
The mechanism of injury is clearly head trauma. All patients with a skull fracture should be evaluated for a concussion, increased ICP, and a cervical spine injury, and treated accordingly. Not all patients with a skull fracture present with a loss of consciousness and not all skull fractures require surgery. Exercise caution during the physical exam to avoid compressing a fractured area and further damaging brain tissue. A fracture in conjunction with an overlying wound, or one that communicates with the paranasal sinuses or middle ear often leads to meningitis. Skull Fracture S/Sx
Skull Fracture Treatment
Looking for a reliable field reference? Consider consider purchasing one of our print or digital handbooks; our digital handbook apps are available in English, Spanish, and Japanese. Updates are free for life. A digital SOAP note app is also available.
0 Comments
You and your partner are planning a two or three day backpacking trip near your home in Boone, NC with your seven year-old daughter and six year-old son. They have been car camping with you for the past three years, taken short day hikes, and enjoyed both. Your daughter is severely allergic to wasps and poison oak; she was hospitalized at four after being stung by a yellow jacket in your backyard. How should you plan your trip? Click here to find out. Don't know where to begin or what to do? Take one of our wilderness medicine courses. Guides and expedition leaders should consider taking our Wilderness First Responder course.
Looking for a reliable field reference? Consider consider purchasing one of our print or digital handbooks; our digital handbook apps are available in English, Spanish, and Japanese. Updates are free for life. A digital SOAP note app is also available. Drowning & Traumatic Injuries While the majority of SUP drowning victims were novices not wearing a life-jacket, at least one drowning victim has died on a river when her leash snagged on hidden debris. Death from head injuries is also a concern when examining surf related accidents. And finally, mild traumatic knee and elbow injuries have occurred in whitewater paddlers. Interestingly, much of the protection available is controversial: The pros and cons of wearing, a leash, helmet, or knee & elbow pads are discussed below. To Wear or Not to Wear...a Leash Purchasing and wearing a leash with your paddle board should NOT be a forgone conclusion but it should be a serious consideration. Your board floats. If you don't wear a life-jacket, you will want to keep your board handy. A leash in flat, calm, protected water, especially for novices, may not be necessary and may well impede learning. On the other hand, wearing a leash while touring, in waves, or surf is usually a pretty good idea and will save you a long swim, or worse, should you fall off your board in heavy surf, strong current, or high wind. Wearing a leash in whitewater is a bit controversial. If you spend a lot of time surfing or running high volume rivers, consider a leash. If you run creeks and small rivers with debris and/or mid-river rocks, you probably shouldn't wear one as it increases your chances of entrapment. If you do choose to wear a leash in whitewater, you'll want one that clips to your life-jacket or waist (not your ankle or knee as these are difficult to reach in strong current), has quick release and break-away functions, and practice using it in strong current. If you choose to wear a leash in flat-water or surf and don't typically wear a life-jacket, you'll likely want one that attaches to your ankle or knee. To Wear or Not to Wear...a Life-jacket While wearing a life-jacket definitely increases your safety, they are somewhat constraining, are hot in the summer, interfere with tan-lines, and are therefore, controversial. Your choice to wear one (or not) depends on your paddling background and your risk assessment: Surfers tend to shun life-jackets and rely on their swimming ability and their board's floatation for protection; whitewater paddlers tend to bring and put on a life-jacket out of force of habit; and novices tend to wear what their instructor or friends wear. Manufacturers try to address comfort via design; inflatable life-jackets stored in belt-packs and activated by a pull-tab are available. No life-jacket will maintain an unresponsive person face up in rough water. NOTE: Many states consider paddle boards a water craft and require operators to either wear a life-jacket or have one on board; some states require board to have lights if used after dark. To Wear or Not to Wear...a Helmet Over the years, people have started to wear helmets in lots of sports where they didn't used to: biking, skate boarding, and skiing to name a few...so why not with an SUP? There have been head injuries and deaths in the surfing community (primarily from hitting their board) yet most surfers shun helmets in the same way they do life-jackets. This trend carries over to SUPs. Conversely whitewater paddlers have grown accustomed to wearing a helmet; after all, if you paddle a kayak or C-1, you are essentially tied into your boat with thigh braces and a spray skirt, and being upside down with rocks coming at your head seems to suggest, even to the most brain dead, that a helmet is a good idea. Again, this trend carries over to SUPs. Flat water canoeists and kayakers typically don't wear helmets (not much momentum if you aren't be pushed around by the water) and, once again, this trend carries over to SUPs. Should you wear a helmet? The answer is easy if you've had a previous head injury and are paddling in surf or whitewater: Wear one. Period. For everyone else, it's controversial. You need to make a personal risk assessment and then a decision. Base both on the likelihood of falling and hitting your head (on the board or something else). The bottom line is that it's safer to paddle with a helmet in the surf and whitewater, than not. To Wear or Not to Wear...Body Armor What? Wear body armor? Are you serious? Well, yes, on whitewater (or if you kneel on your board a lot). If you paddle on shallow rivers or tight rivers with lots of exposed rocks you should consider wearing knee and/or elbow pads. Also consider armored shorts with hip and sacral protection. Having your board stop suddenly after scraping the bottom on a rock tends to toss you forward onto the board or into rocks on the bottom of the river. Most paddlers land hard reasonably hard on their knees, elbows, hips, or back. All are somewhat fragile and hurt considerably when abruptly contacting a rock. Pads protect them. Looking for a reliable field reference? Consider consider purchasing one of our print or digital handbooks; our digital handbook apps are available in English, Spanish, and Japanese. Updates are free for life. A digital SOAP note app is also available.
Introduction Stand up paddle boarding has taken off everywhere there's water: on flat-water, in the surf, and on whitewater. With it come a number of potential problems. Correctly touted as an excellent core workout, a discussion of effective training methods and possible injuries are often overlooked...until something starts to hurt. By then it's too late. Overuse injuries are common. While the overuse injuries in SUP are similar to other paddle sports, they are are exacerbated by the increased leverage of the paddle and the standing position. In order to propel the board forward force must be transmitted from the paddle through the paddler's entire body. Joints are the week points: wrists, elbows, shoulders, back, knees, and ankles. The exact process that makes stand up paddling so good for your core also makes it potentially bad for your joints. There are six things you need to consider when training/paddling SUPs:
Your Paddle You can reduce the strain on your joints by decreasing the length of your paddle, choosing a more flexible paddle shaft, and choosing a small blade size. Decreasing the paddle length directly reduces the size of the lever and therefore the strain on your body. In addition, a shorter paddle lowers your top hand and directly reduces forces on your rotator cuff, shoulder tendons, and cervical spine compression. That said, you don't want a paddle that is too short either as this will cause you to bend over more and increase the strain on your lower back. A flexible paddle shaft absorbs some of the explosive energy during the catch phase of a stroke and spreads the energy release throughout the stroke's length; this dramatically decreases the initial impact on your joints and the potential for damage. Alternatives to carbon-fiber (the stiffest) and fiber-glass blades (next in line) are wood and bamboo. A smaller blade size reduces the surface area of the blade and the amount of energy required for each stroke. While you can purchase smaller blades commercially, you can also cut down the size of your current blade with a jig saw (remember to smooth/sand the edges if you work on your own paddle). Your Body Each individual is unique. Injuries, age, fitness, strength, and flexibility all play an important part in determining what kind of paddling you choose to do and how you approach doing it. For instance, if you have low back problems, it's a better choice to paddle on flat water than in strong whitewater or surf as the sudden movements required for either whitewater paddling or surfing will increase the likelihood of low back injury as you attempt to react to the required changes. Don't ignore your body's history or what it tells you as you paddle and after. Technique Learning the proper paddling technique and paddling on both sides of your board is vital to preventing overuse injuries. Your muscles are designed to be in balance and, in order to prevent injury, you need to keep it that way by learning to paddle correctly on both sides of your board. This may be more difficult that it sounds when surfing or paddling in whitewater as paddlers tend to favor one side or the other. Strength & Flexibility Training If you want to paddle on a regular basis, you'll benefit by spending some time cross-training to avoid injuries. A quick web-search will reveal a number of SUP specific training regimes; one is sure to meet your needs. The Type of Paddling You Do Paddling SUPs on flat-water, in the surf, and on whitewater requires different equipment and skills. The forces on your body are different as well. This means that the types of injuries you can sustain are somewhat specific to the type of paddling you do. Flat-water paddling is typically limited to overuse injuries. While surf and whitewater paddlers are also susceptible to the same overuse injuries as flat-water paddling, moving water is strong and paddling in it increases the chances of muscle and tendon damage; furthermore, traumatic injuries and drowning are also possible. Looking for a reliable field reference? Consider consider purchasing one of our print or digital handbooks; our digital handbook apps are available in English, Spanish, and Japanese. Updates are free for life. A digital SOAP note app is also available.
You are paddling with two friends on the Farmlands section (Class VI-V) of the White Salmon River in Washington state. The day is sunny and 65 degrees F but the water temperature is quite cold at 45 degrees. Most of the river is behind you when one of your friends Jessie, gets offline and runs the slot. Her kayak completely disappears for a few seconds before popping up downstream upside down. There is no sign of Jessie. Chasing her, you see her get scraped out of her boat as it drags over a submerged rock. It takes another 3-5 minutes (?) to rescue her. Once on shore, she is unresponsive, not breathing, and does not have a pulse. You pull her onto a flattish rock and begin CPR. During the second round of chest compressions, a small amount of foam issues from her mouth and nose. You breathe through it. Roughly three minutes later she spontaneously begins breathing. Ten minutes later she is awake and confused with no memory of the event. Her helmet is cracked and her physical exam is unremarkable. She is shivering even though the rock she is on is in the sun; she is wearing a drysuit. Her pulse rate is 52 and regular; her respiratory rate is 16 and easy; her lungs appear dry with no rales, gurgling, or coughing. The Green Truss bridge take out is just downstream and requires ropes to haul your kayaks to the rim. Once at the rim, a clinic is about an hour away and a small hospital an hour further. Jessie wants to get off the water and go home. You have cell coverage. What is wrong with Jessie and what should you do? Click here to find out. Click here to read a blog article on drowning. Don't know where to begin or what to do? Take one of our wilderness medicine courses. Guides and expedition leaders should consider taking our Wilderness First Responder course.
Looking for a reliable field reference? Consider consider purchasing one of our print or digital handbooks; our digital handbook apps are available in English, Spanish, and Japanese. Updates are free for life. A digital SOAP note app is also available. You and two friends are riding an old mountain bike race course when you reach a gnarly downhill section. You elect to slide down the section with your bike and take photos. One of your friends manages to successfully ride down. Unfortunately Jack hits his front breaks too hard, flies over the handlebars landing on his head, neck, and shoulders, then slides with his bike another 50 feet to an open, dry wash at the bottom of the slope. When you reach him, he is sitting up holding his side and having difficulty catching his breath. After a few minutes, he calms down and is able to breath as long as he doesn't try to take a deep breath and breathes with his diaphragm. Jack's helmet is intact and he is able to recall his entire fall. He says he landed hard on his handlebars and thinks he broke a rib low on his left side. Road rash covers most of his back where his jacket slid up during his slide and small pieces of gravel is embedded under portions of his skin; it looks nasty but Jack said it doesn't really hurt. Jack's pulse rate is 88 and regular; his respiratory rate is 22 and easy; he reports that his normal pulse rate is in the low 50s. It's 3 pm, overcast and cool, about 50 degrees F; the sun sets about 7:30 pm. You have a small first aid kit, some water, food bars, but no additional clothing. Nighttime temperatures have been in the low 40s. You are roughly six miles from your vehicles over challenging terrain and another two hours to the nearest clinic. You have cell phone reception. What is wrong with Jack and what should you do? Click here to find out. Don't know where to begin or what to do? Take one of our wilderness medicine courses. Guides and expedition leaders should consider taking our Wilderness First Responder course.
Looking for a reliable field reference? Consider consider purchasing one of our print or digital handbooks; our digital handbook apps are available in English, Spanish, and Japanese. Updates are free for life. A digital SOAP note app is also available. You and one of your friends are thinning trees on a remote piece of property you hope to build on some day. While cutting a leaning tree in some thick brush, Jeep's chainsaw jumped cutting deeply into his left leg. In seconds, his jeans were soaked with blood. You have a couple of tourniquets in your first aid kit along with two hemostatic dressings, gauze, and elastic wraps courtesy of your grandfather. (Too bad you didn't take his advice and purchase protective gear....) Tearing open Jeep's jeans all you see is blood welling up from what appears to be a deep wound. Wiping away the blood with a trauma dressing from the kit, you can see the wound is deep. It quickly filled with dark blood again and direct pressure didn't seem to help very much. Your truck is close by but it's a good four hours to the nearest clinic with no cell reception. What should you do? Click here to find out. Click here to read a blog article on the field management of severe bleeding. Don't know where to begin or what to do? Take one of our wilderness medicine courses. Guides and expedition leaders should consider taking our Wilderness First Responder course.
Looking for a reliable field reference? Consider consider purchasing one of our print or digital handbooks; our digital handbook apps are available in English, Spanish, and Japanese. Updates are free for life. A digital SOAP note app is also available. You are skiing in the backcountry when one of your friends, Jane, catches an edge and crashes into a tree hitting her head—she is wearing a helmet—and upper chest. She is awake, struggling to breathe, and holding her head when you reach her. Her helmet is cracked. After catching her breath, she is confused, has a throbbing headache (6), and doesn't remember her fall, hitting the tree, or the events immediately preceding it. While the left side of her upper chest hurts as you examine her, she is able to take a deep breath without pain. While it is difficult for her to focus during your spinal assessment, she has no spine pain, no mid-line spine tenderness, and normal motor and sensory exams. The rest of her physical exam is unremarkable. Jane plays lacrosse for her college and was hospitalized for a brief period after a concussion three years ago. Her pulse roughly fifteen minutes after the accident was 58 and regular; her respiratory rate 16 and easy; she reports her normal pulse rate is 56. It's a few hours ski to your vehicles, the nearest hospital or clinic is another two hours beyond that, and your cell phone has no bars. There are a total of three people in your party, including Jane. What is wrong with Jane and what should you do? Click here to find out. Don't know where to begin or what to do? Take one of our wilderness medicine courses. Guides and expedition leaders should consider taking our Wilderness First Responder course.
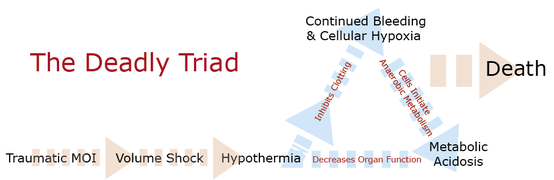
Looking for a reliable field reference? Consider consider purchasing one of our print or digital handbooks; our digital handbook apps are available in English, Spanish, and Japanese. Updates are free for life. A digital SOAP note app is also available. Major traumatic mechanisms often cause life-threatening injuries. If not controlled, those that cause significant internal or external bleeding lead to volume shock and potentially death. It's VITAL that you do everything in your power to keep your patient warm. Here's why: The body responds to blood loss by constricting peripheral blood vessels and increasing their pulse and respiratory rates in an effort to maintain adequate perfusion pressure and a constant supply of nutrients and oxygen to critical organs. As a patient's blood volume drops, their ability to maintain their core temperature also drops and they become increasingly disposed to hypothermia, even in neutral or warm environments. As hypothermia sets in, it interferes with the clotting cascade causing the bleeding to continue further reducing the amount of oxygen reaching the cells. As cells become oxygen-starved, they resort to anaerobic metabolism that ultimately lowers blood pH causing metabolic acidosis that, in turn, damages tissue and organs throughout the patient's body. As organs become damaged, their ability to function also drops, further predisposing the patient to hypothermia. It's a vicious cycle that often ends in death. As such, the importance of keeping trauma patients, especially volume depleted patients, warm cannot be understated. It's important to recognize that injured patients need more insulation—and potentially external heat—than those who are healthy and uninjured; most require a full hypothermia package. That said, be careful not to go overboard and overheat your patient. The skin on their extremities, both hands and feet, should feel warm to the touch when inside the hypothermia package (ensure that your hands are warm); and, if awake, they should not complain of being cold. Looking for a reliable field reference? Consider consider purchasing one of our print or digital handbooks; our digital handbook apps are available in English, Spanish, and Japanese. Updates are free for life. A digital SOAP note app is also available.
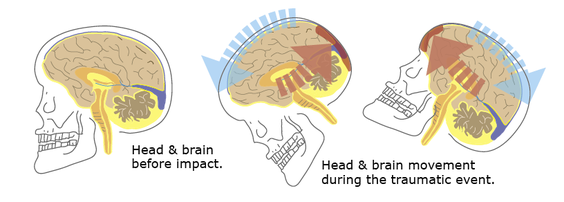
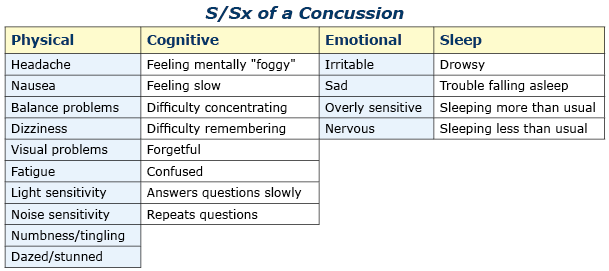
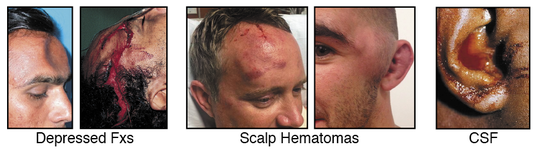
PathophysiologyThe mechanism of injury (MOI) is a direct blow to the patient’s head or a direct blow to another part of their body where the force is transmitted to their brain via their spinal column, cord, and associated soft tissue (aka: whiplash). The brain essentially floats inside the skull in cerebral spinal fluid (CFS). The fluid acts to protect and cushion sensitive brain tissue from minor impacts in much the same way as egg white protects the yolk. If the force generated by the traumatic event is strong enough, the brain will bounce off inside of the skull damaging sensitive brain tissue (as shown in the illustrations below). A concussive injury, should it occur, can be functional or structural. A person with a functional concussive injury will present or develop S/Sx, typically within two hours; however, standard imaging techniques (CT, MRI) show no structural damage. The S/Sx of a functional injury—see the chart below—are likely caused by axional stretching and disruption of ion channels, follow a predefined progression, and usually resolve on their own within 7-10 days; although, in some cases, S/Sx may persist for months. That said, structural damage is possible and may lead to increased intracranial pressure (ICP) and potentially death in rare cases. The concern from a field perspective is whether a person with an apparent positive MOI can remain in the field or requires an evacuation. And, if an evacuation is necessary: What is its urgency? Emergency department physicians typically rely on one of seven clinical algorithms to decide if a patient requires imaging or not (Click here to read an article that discusses the pros and cons of each rule), only the High Risk Criteria for the Canadian CT Head Injury Rule and the NEXUS II can be easily extrapolated to aid evacuation decisions in the field; both may be used in the presence of a significant mechanism of injury. It's important to remember that the guidelines are conservative and few concussed patients go on to develop increased ICP. Assessment All people with a positive mechanism must be evaluated for a potential traumatic brain injury (TBI). TBIs can be grossly subdivided into concussion and increased ICP. Concussions can be further subdivided into mild, moderate, and severe, while increased ICP can be broken down into early and late. After a traumatic MOI a patient may present with any of the problems discussed below and progress, or not, from that point. Note that the problems are mutually exclusive and a patient may only have one problem—concussion or increased ICP—at any given time. Seizures are possible at any point especially in infants and young children and common in unresponsive patients with late increased ICP prior to posturing. Patient's with serious head injuries typically have obvious soft tissue damage to their head including:
Mild Concussion
Moderate Concussion
Severe Concussion The distinction between a moderate and severe concussion is important as the mechanism MAY have been severe enough to structurally injure brain cells or small blood vessels, cause intracranial leaks and swelling, and lead to increased ICP. Worsening S/Sx over the next 24 hours indicate a more severe injury (severe concussion) and can be difficult to recognize if the patient is not closely monitored. Pay close attention to the patient’s overall function: Are their S/Sx severe enough that they interfere with their daily function (severe concussion)? When doubt, choose the worst reasonable case scenario.
Early Increased ICP
Late Increased ICP
Treatment Mild Concussion
Moderate Concussion
Severe Concussion
Early Increased ICP
Late Increased ICP
Looking for a reliable field reference? Consider consider purchasing one of our print or digital handbooks; our digital handbook apps are available in English, Spanish, and Japanese. Updates are free for life. A digital SOAP note app is also available.
|
Categories
All
Our public YouTube channel has educational and reference videos for many of the skills taught during our courses. Check it out!
|

 RSS Feed
RSS Feed
