|
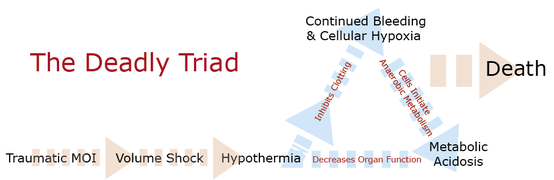
Major traumatic mechanisms often cause life-threatening injuries. If not controlled, those that cause significant internal or external bleeding lead to volume shock and potentially death. It's VITAL that you do everything in your power to keep your patient warm. Here's why: The body responds to blood loss by constricting peripheral blood vessels and increasing their pulse and respiratory rates in an effort to maintain adequate perfusion pressure and a constant supply of nutrients and oxygen to critical organs. As a patient's blood volume drops, their ability to maintain their core temperature also drops and they become increasingly disposed to hypothermia, even in neutral or warm environments. As hypothermia sets in, it interferes with the clotting cascade causing the bleeding to continue further reducing the amount of oxygen reaching the cells. As cells become oxygen-starved, they resort to anaerobic metabolism that ultimately lowers blood pH causing metabolic acidosis that, in turn, damages tissue and organs throughout the patient's body. As organs become damaged, their ability to function also drops, further predisposing the patient to hypothermia. It's a vicious cycle that often ends in death. As such, the importance of keeping trauma patients, especially volume depleted patients, warm cannot be understated. It's important to recognize that injured patients need more insulation—and potentially external heat—than those who are healthy and uninjured; most require a full hypothermia package. That said, be careful not to go overboard and overheat your patient. The skin on their extremities, both hands and feet, should feel warm to the touch when inside the hypothermia package (ensure that your hands are warm); and, if awake, they should not complain of being cold. Looking for a reliable field reference? Consider consider purchasing one of our print or digital handbooks; our digital handbook apps are available in English, Spanish, and Japanese. Updates are free for life. A digital SOAP note app is also available.
1 Comment
jasmine torres
2/25/2019 08:14:16 am
wow this article is so interesting to read, thank you for sharing this post, it was really helpful to read.
Reply
Your comment will be posted after it is approved.
Leave a Reply. |
Categories
All
Our public YouTube channel has educational and reference videos for many of the skills taught during our courses. Check it out!
|
 RSS Feed
RSS Feed
